On a June day in 2012, two elementary school kids in Washington state came home from field day with skin the color of boiled lobsters. Their mom, Jesse Michener, took one look and drove them straight to the hospital. Both girls had albinism, which makes them extremely sensitive to sunlight. They had asked to use sunscreen. The school said no.
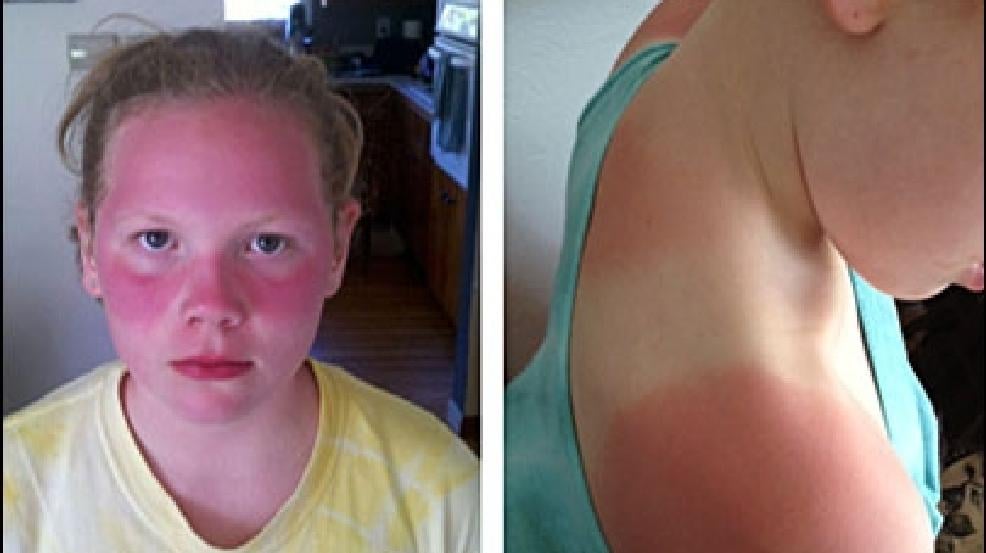
The reason was not malice. It was paperwork. District policy, based on Washington state law at the time, treated sunscreen like a drug. No doctor’s note, no application. So teachers watched kids burn rather than risk violating the rule.
That story sounds bizarre next to another familiar school rule: kids must be vaccinated to attend class. In one case, schools block a basic health measure unless a doctor signs off. In the other, they require a medical intervention unless a doctor signs an exemption. They look similar because both are about kids, consent, and safety. But school sunscreen bans and vaccine mandates grow out of very different histories, methods, and outcomes.
By the end of this comparison, the odd logic of that 2012 sunburn case makes more sense, and so does the way American schools think about risk, liability, and kids’ bodies.
Why did schools treat sunscreen like medicine?
To understand the Washington case, you have to start with a different fear: not sunburn, but allergies and lawsuits.
Through the 1980s and 1990s, American schools were hit with a wave of anxiety over kids having severe allergic reactions to products that adults barely thought about: peanuts, perfumes, latex, and yes, ingredients in lotions and creams. At the same time, parents and districts were increasingly lawsuit-aware. If a teacher gave a child anything that might cause a reaction, the school could be blamed.
States responded by tightening rules on what counted as a “medication” at school. Many state laws and district policies lumped together prescription drugs, over-the-counter painkillers, cough syrup, ointments, and topical products. The logic was simple: if it changes the body in any way, treat it as a drug. That triggered a standard protocol. Parent permission. Often a doctor’s note. Storage in the nurse’s office. Staff training.
In Washington, sunscreen fell into that bucket. The law did not carefully separate an ibuprofen tablet from a bottle of SPF 30. District lawyers, reading the statute, erred on the side of caution. So teachers were not allowed to apply sunscreen to students. In some districts, kids were not even allowed to carry it.
School sunscreen bans came from a risk-avoidance mindset that treated all products with potential side effects as medications that required medical authority.
That is how you end up with a teacher watching a pale child blister in the sun because the law treats sunscreen like a controlled substance. The origin of the sunscreen rule was not health promotion, it was liability management. That starting point shaped everything that followed.
How did vaccine requirements grow out of a different fear?
Vaccine rules in schools grew from the opposite direction. Instead of worrying about a rare allergic reaction, lawmakers were staring at epidemics that killed or disabled kids by the thousands.
In the late 19th and early 20th centuries, American cities were regularly hit by outbreaks of smallpox, diphtheria, measles, and polio. Schools were perfect transmission hubs. Crowded rooms, poor ventilation, and kids who could not easily be kept apart. Public health officials realized that if they could raise immunity in schools, they could slow or stop citywide outbreaks.
By the early 1900s, some cities, like Boston and New York, began requiring smallpox vaccination for school attendance. Parents sued, arguing that compulsory vaccination violated personal liberty. In 1905, the U.S. Supreme Court decided Jacobson v. Massachusetts, upholding a state’s power to require vaccination during a smallpox outbreak. That case became the legal backbone for school vaccine mandates.
Over the 20th century, as new vaccines were developed, states added them to school entry requirements: diphtheria, tetanus, pertussis, polio, measles, mumps, rubella, and more. By the 1980s, all 50 states had some form of school vaccination law.
School vaccine mandates were designed as a public health tool to prevent deadly outbreaks, not as a liability shield. The core fear was contagious disease, not lawsuits. That origin made schools comfortable doing something they would never do with sunscreen: requiring a medical intervention as a condition of attendance.
So what? The starting fears were different. Sunscreen rules grew from fear of individual adverse reactions and legal blame, while vaccine mandates grew from fear of epidemics and mass illness. That difference explains why one policy blocks a health measure without a doctor, and the other enforces one unless a doctor objects.
How do the methods differ: permission vs obligation?
Once you see the origins, the methods fall into place. Sunscreen policies and vaccine mandates use opposite default settings.
With sunscreen in many states before 2012, the default was no. A child could not use or receive sunscreen at school unless adults jumped through specific hoops. Parents had to provide the product. Often they needed a doctor’s note. Staff had to follow storage and application rules. If any step failed, the answer reverted to no.
Teachers were also told not to touch students in ways that might be construed as inappropriate. Rubbing lotion on a child’s shoulders or legs fell into a gray area. So even when rules technically allowed sunscreen with paperwork, many staff avoided applying it. The safest choice, from a job-security perspective, was to refuse.
Vaccines flipped that script. The default is yes. To enroll in public school in most states, a child must show proof of certain vaccinations. Parents do not need to request the rule. They must comply with it or seek an exemption. The burden is on the family to opt out, not on the school to justify opting in.
There is also a timing difference. Sunscreen is an on-site intervention. It happens at school, in real time, under staff supervision. Vaccination is an off-site intervention. It usually happens in a clinic, long before the child walks into the classroom. Schools check paperwork, not needles.
That distinction matters legally. When a teacher applies sunscreen, the school is directly involved in the act. If something goes wrong, the school is on the hook. When a school checks a vaccine record, it is enforcing a law, not administering medicine. The medical act happened elsewhere, under a doctor’s license.
So what? Sunscreen rules make schools gatekeepers of on-site medical acts, so they default to blocking anything without explicit authority. Vaccine rules make schools paperwork enforcers for off-site medical acts, so they default to requiring them unless an exemption is granted. The methods reflect who is touching the child and when.
What were the outcomes: sunburns vs herd immunity?
By 2012, the sunscreen-as-medication approach had a visible cost. Kids got burned.
Jesse Michener’s daughters were not the only ones. Dermatologists had been warning for years that children were getting serious sunburns at school events because they were not allowed to apply sunscreen or wear hats. Some kids, like Michener’s, had conditions that made them especially vulnerable. Others simply spent hours outside with no shade and no protection.
Parents were furious when they learned why. The idea that a child could be hospitalized for sunburn because a school needed a doctor’s note for a bottle of SPF 50 sounded absurd. Stories like the Washington case spread online and in local news. They made the trade-off visible: in trying to avoid rare allergic reactions and legal risk, schools were causing frequent, predictable harm.
Vaccination rules, by contrast, produced quieter, statistical outcomes. When vaccine coverage in schools is high, disease outbreaks shrink or vanish. Measles cases in the United States plummeted after widespread vaccination and school mandates. Polio disappeared from American classrooms. Most parents today have never seen a child in an iron lung or a classroom closed by diphtheria.
There are side effects and rare adverse events from vaccines, and those have fueled debate and resistance. But from a population perspective, the outcome of school vaccine mandates has been fewer hospitalizations and deaths from infectious disease.
So you end up with a strange contrast. The sunscreen rule produced visible, immediate harm to individual kids in the name of preventing rare reactions. The vaccine rule produced invisible, long-term protection for many kids while accepting a small, monitored risk of side effects.
So what? Sunscreen bans made harm obvious and personal, which sparked outrage and quick policy change. Vaccine mandates made benefit widespread and statistical, which made them easier to defend in law but harder for some people to emotionally grasp.
How did the Washington sunburn case change sunscreen laws?
The 2012 Washington incident did not stay a local embarrassment. It turned into a policy lesson.
After Michener wrote publicly about her daughters’ burns, the story hit national media. Parents and doctors pointed out that every major cancer and dermatology group recommends sunscreen for kids during prolonged sun exposure. The American Academy of Dermatology had long argued that sunscreen should be treated as basic sun safety, not as a restricted drug.
Lawmakers in Washington took notice. In 2017, the state passed a law allowing students to bring and apply sunscreen at school without a doctor’s note. Other states, including California and Oregon, had already moved in that direction or followed soon after. Many districts updated their policies to make sunscreen an exception to the general medication rules.
Some schools went further. They added shade structures to playgrounds. They encouraged hats and long sleeves. They trained staff to remind kids to apply sunscreen before outdoor events. The idea shifted from “we might get sued if a child has a reaction” to “we might get sued if we knowingly let a child burn.”
In short, the Washington case helped push sunscreen into the category of routine, low-risk self-care, like drinking water, rather than high-risk medication.
So what? The public backlash to the sunburn case forced lawmakers to recalibrate their risk calculus, moving sunscreen from a tightly controlled medical item to a basic safety tool that kids can use without jumping through medical hoops.
Why have vaccine mandates been harder to change?
While sunscreen rules shifted quickly after a few high-profile cases, vaccine mandates have been far more stable, even in the face of vocal opposition.
Part of that is legal. School vaccination laws rest on more than a century of court decisions affirming states’ power to protect public health. When parents challenge mandates, courts usually side with the state, especially when exemptions exist for medical reasons and sometimes for religious or philosophical ones.
Part of it is epidemiology. When vaccine coverage drops, outbreaks follow. In the late 2010s, areas with low measles vaccination rates saw clusters of cases. Public health officials could point to a clear cause-and-effect: fewer vaccinated kids, more disease. That feedback loop reinforces the idea that school mandates work.
There is also a structural difference. Changing a sunscreen policy often requires a school board vote or a tweak to a state education rule. Changing vaccine mandates usually means amending state law, taking on organized advocacy groups, and confronting national debates about bodily autonomy and distrust of pharmaceutical companies.
So while sunscreen rules bent quickly under the weight of a few dramatic stories, vaccine rules have held because they are backed by long-term data, legal precedent, and the memory, at least among older generations, of what life was like before vaccines.
So what? Sunscreen policy was a relatively low-stakes, low-friction fix once the harm was visible, while vaccine mandates are tied into deep legal, political, and scientific structures that make them far harder to unwind.
What is the legacy of these two school health rules?
Today, in many states, a child can carry a small bottle of sunscreen in their backpack and apply it before recess without involving a nurse or a doctor. That shift traces directly back to cases like the 2012 Washington sunburns, where the absurdity of the old rule became impossible to ignore.
The legacy of the sunscreen debate is a reminder that overprotective policies can backfire. Treating every health product as a legal hazard can cause the very harm the rules were meant to prevent. It also shows how a single vivid story, amplified by social media, can push lawmakers to redraw the line between caution and common sense.
Vaccine mandates, on the other hand, remain a central part of how American schools manage public health. They are not perfect. They are contested. But they have helped turn once-common childhood killers into rare news stories. Their legacy is measured not in dramatic Reddit posts, but in the quiet absence of disease.
They look similar because both sunscreen bans and vaccine requirements involve schools, kids, and questions of consent. Underneath, they are different species of policy. One grew from fear of liability and was trimmed back when that fear caused obvious harm. The other grew from fear of epidemics and has endured because the harm it prevents is far greater than the risk it carries.
So the next time a school note comes home about sunscreen or shots, it is not just bureaucracy. It is a small piece of a long argument over who protects children’s bodies, and how much risk we are willing to accept to keep them safe.
Frequently Asked Questions
Why did some schools ban sunscreen without a doctor’s note?
Many states and school districts used to classify sunscreen as a medication, just like painkillers or ointments. That meant students could not use it at school without parent permission and often a doctor’s note. The rules were written to avoid allergic reactions and lawsuits, but in practice they left some kids unprotected and led to cases of severe sunburn.
What exactly happened in the 2012 Washington sunscreen incident?
In 2012, two elementary school students in Washington state, both with albinism, participated in a field day and were not allowed to use sunscreen because they did not have a doctor’s note on file. They suffered severe sunburns and were taken to the hospital by their mother, Jesse Michener. The school district said its policy followed state law that treated sunscreen as a medication.
How are school vaccine requirements different from sunscreen rules?
School vaccine requirements are state laws that require children to be vaccinated against certain diseases before attending school, with limited exemptions. Vaccination usually happens off-site at a clinic, and schools check records. Sunscreen rules were local or state policies about what staff could apply on-site during the school day. Sunscreen was restricted to avoid liability, while vaccines are required to prevent disease outbreaks.
Did the Washington sunburn case change sunscreen laws?
Yes. Public outcry over cases like the 2012 Washington incident pushed lawmakers to change policies. In 2017, Washington passed a law allowing students to carry and apply sunscreen at school without a doctor’s note. Other states have made similar changes, treating sunscreen as basic sun protection instead of a restricted medication.